Did you know that in the Finnish language, there is at least 13 different words to describe snow? “Lumi” is the general word for snow but soft, dry, newly fallen snow is called “viti” and moist snow that is suitable for making a snowman is called “nuoska.” Depending on the water content, really wet snow is called “loshka” but wet snow with a lesser amount of water is called “sohjo.” I think it’s fascinating that in other cultures, they need different words to describe things with subtle complexities.
Apart from cancer, when it comes to the musculoskeletal system, there are 2 words that are often used that unfortunately, tends to provoke anxiety and fear in people: the words “tear” and “degeneration.” We have no other words to describe the nuances of these conditions. The former relates to our soft tissues like muscles, ligaments and tendons. The latter is often used to describe bones and joints. This limitation of the English language unfortunately, is not helpful.
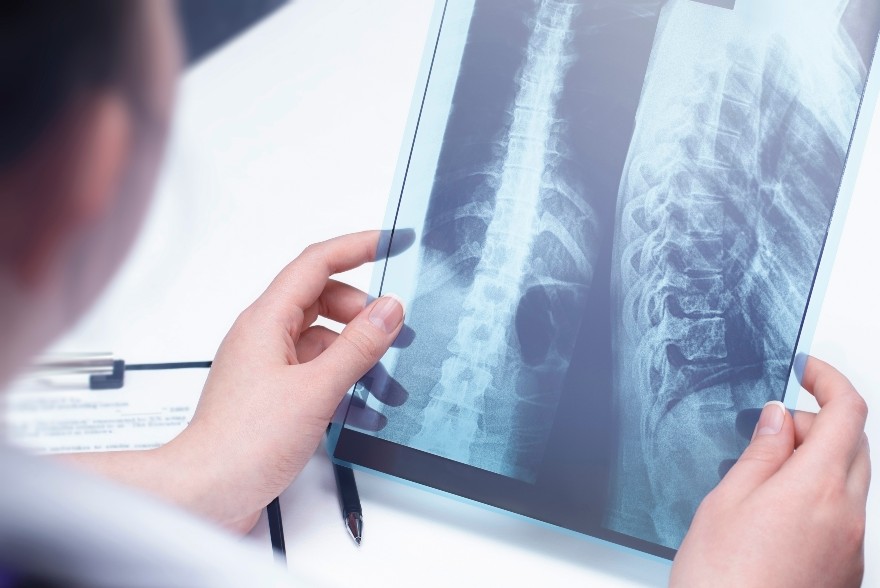
There are so many reasons why muscle and joints can show changes on radiological tests like Xrays and ultrasound. As humans age, our soft tissue and bones/joints will demonstrate natural age-related changes that is often asymptomatic. Like beautiful wrinkles on our skin and gray hair, many of these findings are not pathological, painful or progressive. It’s just a snapshot of our age. And yet, if an ultrasound is done on these soft tissues and if an Xray is done on our spines, it is unfortunate that the only words we have to describe these findings are the words “tear” and “degeneration.” It is what we associate these words to mean that is not helpful because of the fear it brings to movement. It also does not answer the following questions:
- Are the findings new or have they been present for years? In other words, is the finding really the problem or is it a natural age-related observation?
- How relevant is the finding and is it even responsible for my symptoms?
How do we answer these questions? In musculoskeletal management, radiology like Xrays, ultrasound and MRIs are helpful but they should not be relied on solely for proper management. Current best practice guidelines for non-traumatic shoulder pain, for example, does not require radiology before the initiation of rehabilitation like physiotherapy. The decision to proceed to radiology requires careful and intentional clinical decision making and when performed, the findings have to be interpreted carefully with the clinical presentation of the patient. This is the only way to know how any radiology findings relate to one’s clinical presentation.
With all this as our context, let’s answer some of your most common questions as it pertains to shoulder rotator cuff injuries and low back osteoarthritis:
Question 1: I have a rotator cuff tear on ultrasound. Do I need surgery?

Shoulder pain is a very common complaint seen in both physician’s offices as well as physiotherapy clinics, increasing in prevalence due to an ageing population (1). Rotator cuff tears are among the most common causes of pain and dysfunction in the shoulder, and typically increase in incidence with age (1). They can occur from an acute injury, or develop without any reason or injury.
There have been many studies that have shown that rehabilitation can be very successful in managing rotator cuff tears and shoulder pain (1,2,3). Interestingly, some studies have shown that anywhere from 5% to 40% of people without any shoulder pain at all have a tear of their rotator cuff (1,2,3). Many studies have compared surgical intervention to conservative management and have found similar gains in function and pain relief at the 12 month mark post injury (2,3). Typically, unless the tear resulted from trauma and results in a complete inability to lift the arm, the current recommendation is to trial 12 weeks of rehabilitation before considering more invasive management (4). If pain is limiting progress with rehabilitation, sometimes a cortisone injection may help reduce barriers to recovery (4).
Question 2: I have osteoarthritis in my low back. I can’t imagine how Physiotherapy and exercise can help my pain since the arthritis is permanent.

Degeneration of the lumbar intervertebral discs, bulging, and facet joint arthropathy (joint changes) have been documented in almost 90% of asymptomatic patients over 60 years of age. After the age of 40 years, nearly all patients have anterior and lateral vertebral osteophytes or bone spurs (5). What the Xray does not tell you is how long the arthritis has been present and how much it is actually contributing to your symptoms. The arthritis itself may not be relevant, as your pain generator may be stemming from other sources. Even if the pain generator is coming from your low back, the Xray does not tell us the reason for the symptom onset and perpetuation. Maybe the ligaments are being irritated from a poor sitting posture. Maybe a lack of hip strength on one side is placing a greater weight bearing load on the low back joints. Maybe changing the way you lift will reduce the repetitive load on a particular part of your spine, thus solving the problem. If these age-related changes have nothing to do with your pain, then “osteoarthritis” is not the cause of your problem.
If you have had Xrays, ultrasound or MRI findings of your condition and if you have questions or concerns about their findings, always discuss these with a health care practitioner who understands your condition. Correlating these findings with your actual clinical presentation is key.
References:
(1). Edwards, P et al. Exercise Rehabilitation in the non-operative management of rotator cuff tears: A review of the literature. International Journal of Sports Physical Therapy 2016 11(5). 279-301.
(2). Ranebo, M et al. Surgery and physiotherapy were both successful in the treatment of small, acute, traumatic rotator cuff tears: A prospective randomized trial. Journal of Shoulder and Elbow Surgery 2020 29, 459-470.
(3). Kuhn, J, et al. Effectiveness of physical therapy in treating atraumatic full-thickness rotator cuff tears: a multicenter prospective cohort study. Journal of Shoulder and Elbow Surgery 2013 22, 1371-1379
(4) Alberta Bone and Joint Health Institute: Shoulder Assessment Clinical Pathways. May 2022
(5) Wocial K, Feldman BA, Mruk B, Sklinda K, Walecki J, Waśko M. Imaging features of the aging spine. Pol J Radiol. 2021 Jun 28;86:e380-e386. doi: 10.5114/pjr.2021.107728. PMID: 34322188; PMCID: PMC8297484.
Submitted by Danielle Bles and Albert Chan

